Mortuaries
Contents
- 1 OVERVIEW
- 2 LEGISLATIVE CONTEXT
- 3 SERVICE CONTEXT
- 4 PLANNING AND DESIGN
- 4.1 Introduction
- 4.2 Location of the Mortuary and Access Routes
- 4.3 Facility Capacity
- 4.4 Selecting Body-Storage Systems
- 4.5 Facility Layout
- 4.6 Mortuary Equipment Requirements
- 4.7 Movement Within a Mortuary
- 4.8 Services Required
- 4.9 Biological Safety
- 4.10 Finishes to Floors and Walls
- 4.11 Autopsy Equipment/Fixtures
- 4.12 Ventilation
- 4.13 Air Conditioning
- 4.14 Refrigeration Equipment Design and Installation
- 4.15 Security Arrangements
- 5 OPERATION
- 6 ROOM USER REQUIREMENTS
- 7 EXAMPLES AND CASE STUDIES
OVERVIEW
This document outlines the policy and service context and attempts to illustrate the desired planning principles and design considerations for mortuary services.
LEGISLATIVE CONTEXT
The following documents, as amended (though not an exhaustive list) pertain and contain an additional resource of information which would supplement and provide the basis of a design brief. A finer sense of standard operating procedures and legislative context is likely to inform and enhance the design process, so the professional teams are encouraged to use these as an additional resource:
- Births and Deaths Registration Act 1992. (c.51).Cape Town South Africa: Government Gazette.
- Criminal Procedure Act 1977.(c.51).Cape Town South Africa: Government Gazette.
- Department of Environmental Affairs and Development Planning Western Cape Province,2004. Western Cape health care waste management draft bill.(P.N.255/
2004). Province of Western Cape South Africa: Provincial Gazette.
- Department of Health (DoH),2013.Regulations relating to the management of human remains. (Government notice No.R.363 of the National Health Act,2003.(c.61).South Africa: DoH.
- Department of Public Works,2005.Space planning norms and standards for office accommodation used by organs of state. (Government notice 1665).Cape Town South Africa: Government Gazette.
- Health Professions Act of 1974. (c.56).Cape Town South Africa: Government Gazette.
- Inquests Act 1959.(c.58).Cape Town South Africa: Government Gazette.
- Municipal By-laws, as applicable
- National Archives of South Africa Act 1996. (c.42).Cape Town South Africa: Government Gazette.
- National Code of Guidelines for Forensic Pathology Practice in South Africa,20 Aug 2007
- National Environmental Management: Waste Act 2008. (c.59).Cape Town South Africa: Government Gazette.
- National Health Act 2003.(c.61).Cape Town South Africa: Government Gazette.
- Standard Operating Procedures, Forensic Pathology Service, PGWC DoH,2006
- U.S.Department of Health and Human Services, Public Health Service, Centers for Disease Control and Prevention and National Institutes of Health,2007.Biosafety in microbiological and biomedical laboratories. (Fifth Edition)..Atlanta Georgia USA: U.S.Department of Health and Human Services.
- University of Pretoria (UP) in partnership with Southern African Legal Information Institute (SAFLII),2012.Regulations relating to the registration of microbiological laboratories and the acquisition, importation, handling, maintenance and supply of human pathogens.(Government notice No.R.178 of the National Health Act,2003.(c.61). Cape Town South Africa: Government Gazette.
- University of Pretoria (UP) in partnership with Southern African Legal Information Institute (SAFLII),2007.Regulations regarding the rendering of forensic pathology service.(Government notice No.R.636 of the National Health Act,2003.(c.61).Cape Town South Africa: Government Gazette.
Infection Prevention and Control Legislation
The National Infection Prevention and Control Policy and Strategy document makes specific reference to certain Acts and their relevant regulations, which bear relevance to the development and implementation of these health facility guidelines. These are:
- Constitution of the Republic of South Africa,1996. s.2,24,27,36&39.
- Department of Health,2003.Regulations relating to the application of the hazard analysis and critical control point system (HACCP system).(Government notice No.R.908 of the Foodstuffs, Cosmetics and Disinfectant Act,1972.(c.54)).Cape Town South Africa: Government Gazette.
- Department of Labour,2001.Regulations for hazardous biological agents. (Government notice No.R.1390 of the Occupational Health and Safety Act,1993.s.43).Pretoria South Africa: Government Gazette.
- The Environmental Conservation Act 1989. (c.73).Cape Town South Africa: Government Gazette.
- The Foodstuffs, Cosmetics and Disinfectants Act 1972. (c.45).Cape Town South Africa: Government Gazette.
- The Occupational Health and Safety Act 1993.s.8(1).Cape Town South Africa: Government Gazette.
Building Legislation
The following legislation and regulations impact and provide guidance on the provision and design of health care facilities as above:
- Building Regulations and Building Standards Act 1977.(c.103).Cape Town South Africa: Government Gazette.
- Promotion of Equality and Prevention of Unfair Discrimination Act,2000.(c.4).Cape Town South Africa: Government Gazette.
- South African Bureau of Standards (SABS),1986.SABS 1200 A-1986 Standardized specification for civil engineering construction.Pretoria South Africa: SABS Standards Division.
- South African Bureau of Standards (SABS),1992.SABS 0100-1 The structural use of concrete Part 1: Design.Pretoria South Africa: SABS Standards Division.
- South African Bureau of Standards (SABS),1992.SABS 0100-2 The structural use of concrete Part 2: Materials and execution of work.Pretoria South Africa: SABS Standards Division.
- South African Bureau of Standards (SABS),1993.SABS 0160 General procedures and loadings adopted in the design of buildings.Pretoria South Africa: SABS Standards Division.
- South African Bureau of Standards (SABS),2010.SANS 10400-A: 2010 The application of the national building regulations Part A: General principles and requirements.Pretoria South Africa: SABS Standards Division.
- The National Environmental Management Act 1998.(c.107). Cape Town South Africa: Government Gazette.
South African Building Practice Policy and Guidelines
- Department of Health (DoH),1980.Regulations governing private hospitals and unattached operating theatres. (Government notice No.R.158 of the Health Act,1971.(C.63).Cape Town South Africa: Government Gazette.
- The South African Pharmacy Council,2004.Good pharmacy practice.(Board notice 129).Cape Town South Africa: Government Gazette.
International Design Guidance
- American Society of Heating, Refrigerating and Air-Conditioning Engineers (ASHRAE),1999.ANSI/ASHRAE standard 52.2-1999 Method of testing general ventilation air-cleaning devices for removal efficiency by particle size.Atlanta USA: ASHRAE.
- American Society of Heating, Refrigerating and Air-Conditioning Engineers (ASHRAE),1989.ASHRAE standard 62 Ventilation for acceptable indoor air quality.Atlanta USA: ASHRAE.
- American Society of Heating, Refrigerating and Air-Conditioning Engineers (ASHRAE),2003.HVAC design manual for hospitals and clinics.Atlanta USA: ASHRAE.
- American Society of Heating, Refrigerating and Air-Conditioning Engineers (ASHRAE),2009.ANSI/ASHRAE/ASHE standard 170-2008 ventilation of health care facilities.Atlanta USA: ASHRAE.
- Chartered Institution of Building Services Engineers (CIBSE),1997.CIBSE applications manual AM10 natural ventilation in non-domestic buildings.London: CIBSE.
- Chartered Institution of Building Services Engineers (CIBSE),2000.CIBSE applications manual AM13 mixed-mode ventilation.London: CIBSE.
- Department of Health and Human Services (Center for Disease Control and Prevention),2003.Environmental control for tuberculosis: Basic upper-room ultraviolet germicidal irradiation guidelines for healthcare setting.USA: DHHS.
- QASA.“Know Your Rights” [Accessibility & the Built Environment]
- World Health Organisation (WHO),2009.WHO policy on TB infection control in health-care facilities, congregate settings and households.Geneva Switzerland: WHO.
- Guidance has also been provided by AIA (USA), NHS (UK), and Australian Health Facility Guidelines on Healthcare Building Design.Additional references can be sourced from www.tb-ipcp.co.za
Further reference material and precedent
- Australasian Health Infrastructure Alliance (AHIA),2007.Australasian health facility guidelines: Part B: Health facility briefing and planning.[online] New South Wales: AHIA.Available at: |AllItems.aspx Accessed 4 March 2014.
- Department of Public Works (DPW),1998.Fire security: A guide for architects. (Ref: F.P.O./G.61/3E).South Africa: DPW.
- Department of Public Works (DPW),1998.Standard specification for air-conditioning and ventilation installations. (PW 327).South Africa: DPW.
- Department of Public Works (DPW),2004.Standard electrical specifications. (PW 354).South Africa: DPW.
- NHS Estates,2001.Health Building Note (HBN) 20: Facilities for mortuary and post-mortem room services.Norwich England: The Stationery Office (TSO).
- South African Bureau of Standards (SABS),2013.CKS 336:2013 Mortuary trolleys.Pretoria South Africa: SABS Standards Division.
SERVICE CONTEXT
| Service | District | Regional | Tertiary | Central | Specialised |
|---|---|---|---|---|---|
| Small (beds) | 50-150 | Min 300 | Min 400 | - | - |
| Medium (beds) | 150-300 | - | - | - | - |
| Large (beds) | 300-600 | Max 800 | Max 800 | Max 1200 | Max 600 |
| Training | Where practical | Where practical | Optional | Yes. (Attached to medical school) |
|
| Conduct research | Yes | ||||
| Mortuary | |||||
| Short-term stay (+2˚C) | Yes | Yes | Yes | Yes | |
| Long-term stay (-20˚C) | Yes | Yes | Yes | Yes | |
| Autopsies (20°C -21°C) | Yes | Yes | Yes | Yes | Yes |
For the determination of capacity requirements of mortuaries refer to the recommendations further on in this guide.
This guidance document relates to mortuaries located within and serving hospitals, with respect to persons that die due to natural causes in that hospital.
This guidance excludes mortuaries dealing exclusively with cases that require medico-legal investigation of deaths from unnatural causes.
Post mortems conducted in hospital mortuaries should be limited to conducting investigations and procedures where no medico-legal investigation is required and death from natural causes is suspected.
Hospital deaths from natural causes and those suspected to be of unnatural cases should not be managed in the same facility unless the hospital mortuary is equipped to comply with the specific staffing infrastructure and operational requirements as they relate to the legislated forensic pathology services mandates, etc.
The requirements for forensic-pathology service mortuaries are not exhaustively detailed in this document.
It is also noted that some hospitals may opt to contract out the removal and storage of decedents to private undertakers and these hospitals may require only the minimum in terms of refrigerated body storage.
PLANNING AND DESIGN
Introduction
- All state-run mortuary facilities fall within the domain of the Department of Health, both National and Provincial; and in an effort to provide engineers and architects who are required to either design new facilities or upgrade existing facilities, this document provides the minimum standards necessary to comply with existing legislation.
- This document will provide designers of this type of facility with guidelines as to what is required in terms of the following:
- Type of service and package of care being provided
- Mortality rate
- Access and egress
- Discreet management of human remains
- Size and dimensions of the actual facility
- Positioning of mortuaries within hospitals
- Finishes of surfaces in these facilities
- Water-supply requirements
- Drainage requirements
- Electrical supply and lighting requirements
- Installation requirements for equipment and services
- Body-storage requirements
- Body-handling facilities
- Body-holding areas
- Body-viewing area
- Autopsy equipment (tables)
- Air conditioning and ventilation requirements (for infection and indoor air quality control)
- Security of the facility
- In addition to the items listed above, it is also necessary to consider the needs of visitors to these facilities, particularly those wishing to, or who are required to, identify bodies. In line with this, it is also necessary to take the handling of bodies into consideration as it pertains to issues of patient dignity.
- Forensic pathology mortuaries are not exhaustively described in this document, although the majority of hospital mortuaries do have basic facilities for general autopsies that are not medico-legal in nature. A forensic pathology service mortuary has laboratory facilities attached, as well as legislated operational requirements that are outside the scope of regular mortuaries found in hospitals. It should be noted that there are a number of principles that hold true for both hospital and forensic pathology mortuaries.
- Compliance with the requirements of the Occupational Health and Safety Act (Act 85 of 1993 as amended) are to be complied with at all times during the design of a mortuary.
Location of the Mortuary and Access Routes
The position of the mortuary in a hospital should be such that the mortuary is easily accessible to mortuary staff and related service providers without presenting either aesthetic, emotional or ethical problems for unrelated hospital staff, patients or visitors. Visitors to the mortuary, however, should be provided with clear and direct access to the mortuary upon arrival at the hospital, without having to travel unnecessarily through hospital departments.
Where bodies are moved into or out of the mortuary, they should not be moved through general public-access areas. Appropriate routes would include technical service or goods corridors and through the hospital’s support services yard.
Special considerations should be given to plans for contingency access to the mortuary in the event of case-load surges, which may result from disasters.
Bodies should not be held for any period in any locations between the body-holding rooms within clinical areas and the mortuary.
Where a mortuary unit is used jointly between the hospital and the local authority it is beneficial for the mortuary to be in a building separate from the main hospital building.
The delivery of bodies to the mortuary and their subsequent removal from the facility is to be such that it is carried out in a manner that is not visible to the general public, preferably in a covered and enclosed area.
While siting and access are important aspects when locating a mortuary, it is also important to provide the mortuary with pleasant surroundings in order to promote the dignity of those working in or visiting the mortuary.
Facility Capacity
The layout and size of a mortuary is largely determined by the number of bodies stored and whether body storage needs to be in cabinets or in refrigerated rooms.
In order to determine the storage capacity of a hospital mortuary, it is recommended that historical data, where available, should be used. In the South African context, it is suggested that a storage capacity of between 5 and 10 bodies per 100 beds should be used. This varies with the rural or urban location of the facility. This capacity should not take into account the need to store bodies from deaths which are not hospital-related, typically motor-vehicle accident deaths and deaths from criminal activity. Requirements for contingency storage capacity related to disaster management should be considered.
The body storage capacity required can be estimated on the basis of the number of deaths per year in the hospital, the length of time of holding and the required body store occupancy rate.
The number of body trays can be calculated from the equation:
BT=(D×S)/(365×R)
Where:
BT = Number of body trays
D = Number of deaths per year requiring body trays
S = Average length of stay (in days)
R = Required body tray occupancy rate
| Example |
|---|
The number of body trays required in a hospital that records 800 deaths per year (not necessarily all within the hospital per se but including bodies delivered to the hospital), with the average length of time that a body remains in the mortuary being 8 days and with a body tray occupancy rate of 80%.
BT = (D x S) / (365 x R) = (800 x 8) / (365 x 0.8) = 6400 / 292 = 21.92 With body cabinets generally having a storage capacity of three bodies per cabinet the calculated required capacity should be rounded up to the nearest multiple of three and as such in the above example 8 cabinets would be required. |
The estimated storage capacity for bodies in a mortuary could be confounded by a number of local factors, such as:
- Mortality rate from natural causes.
- Mortality rate from infectious disease.(Highly contagious disease deaths require special storage facilities.)
Where the hospital is expected to place the body in cold storage until collection by forensic pathology services, the following additional factors should be considered with respect to numbers of unnatural deaths (accidental, suicidal, homicidal, unknown and procedure-related deaths) anticipated at any particular hospital, including:
- Mortality rate from foul play (homicide) or suicide
- Mortality rate from traffic or other accidents
- Mortality rate from procedure-related deaths
- Mortality rates from sudden, unexpected or unexplained deaths
Selecting Body-Storage Systems
Body-storage systems are principally divided into refrigerated rooms or body cabinets. Differences within these system types occur where specific temperatures or sizes are required based on risk, need and capacity requirements. Body cabinets should be arranged such that the lowest shelf would have sufficient capacity for the heaviest bodies.
Where a system of functionally separate body cabinets is selected, this system would have an inherent redundancy against failure, as the failure of a single unit would not necessarily imply a system failure. In contrast, a refrigerated room would require less maintenance and would have a lower frequency of failure; however, a single component failure could be critical if standby condensing units are not installed. For this reason,multiple-cabinet systems are recommended for areas where expected maintenance response times would negatively affect the mortuary’s operations.
It is possible to have a requirement for a mixture of refrigerated rooms and body cabinets. This could be affected by local cultural requirements such as for families who object to bodies sharing storage space, the caseload of the facility or the case profile.
Where there is a requirement for the long-term storage of bodies, these are to be kept at a lower temperature than would be the case in a refrigerated room. In this instance, separate body cabinets are required. Long-term storage of bodies is most often required when an indigent person dies and difficulty is experienced in locating the next of kin, as the person cannot legally be buried until this process has been completed.
In general, smaller facilities rely on body cabinets for the storage as these facilities do not have the space or the need for the large-scale storage of bodies, they would not appreciate the functional flexibility offered by these systems. By rule of thumb, any facility that has the requirement to store fewer than 12 bodies at any given time should use body cabinets. This gives the option of providing both short- and long-term storage with the smallest facility and equipment footprint.
Bodies suspected of having succumbed to a highly contagious and dangerous disease require special treatment. These should be stored in such a manner that they do not present a hazard to personnel working in the mortuary. Typically these bodies should be stored at the same temperature as long-stay bodies,e.g.-20°C, and should be placed in hermetically sealed plastic body-bags.
Provision for the secure cold storage of body parts should be provided.
Facility Layout
As mentioned, the layout and size of a mortuary are going to be largely determined by caseload and whether storage is in cabinets or refrigerated rooms. It is acceptable to have a mixture of refrigerated rooms and body cabinets.
In a mortuary facility, there are a number of separate areas that need to be considered other than the body-storage areas. These include:
- Reception area for members of the public who are required to visit the mortuary on official business – typically to identify bodies or to pay their last respects to a deceased person.
- Ablution areas for staff. Where unisex ablutions are provided it is recommended that no urinal is provided.
- Visitors’ admin space close to the reception area, where any admin or official business related to the identifying of a body can be completed.
- Staff admin space close to the point where a body is delivered to the mortuary so that pertinent documentation can be completed – both with respect to the delivery of the body, as well as when the body is released from the mortuary again.
- Office space for pathologists to write up reports in instances where this could be required. This is dependent on the size of the mortuary as small facilities would not require a separate room(s) for this function.
- Waiting and circulation areas for visitors to the mortuary.
- Viewing room, from where a body can be viewed through a curtained glass window between this space and the body-display room.
- Body-display room, where a body is placed for identification purposes. There is to be access to this area via a lockable door to the viewing room in instances where it is necessary for non-mortuary personnel to have direct access to a body in the viewing room. There is to be access to this room from the body-storage area to allow bodies to be brought in for display purposes.
- Body preparation area, where a body that is delivered to the mortuary needs to be attended to prior to it being placed in the viewing room.
- Shower facilities (staff)
- Changing room (staff)
- Storage space for equipment and clothing that is worn in the body-preparation and autopsy spaces.
- Body-storage facility (cold room or refrigerated cabinets), depending on the length of time that bodies are expected to be kept in the facility.
- Autopsy facility, where the cause of death can be determined. This facility will differ from mortuary to mortuary, depending on whether forensic pathology service or standard medical autopsies to determine the cause of death are conducted.
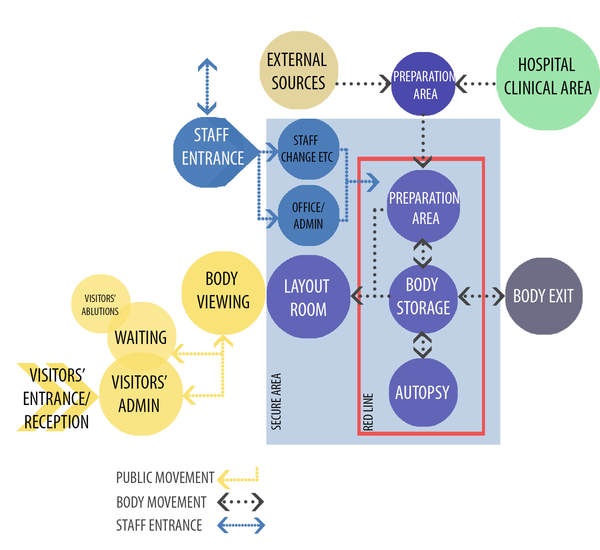
- The image below is an example of an adjacency diagram for a typical mortuary. In this instance, the proximity also relates to visual and physical access. It is also understood that not all mortuaries would require all of the spaces indicated in this diagram and that some of the spaces shown as being immediately adjacent could be included as a single area should functionality and privacy considerations permit it.
- There remains abundant scope for variations in the planning of the layouts making up the mortuary. The hospital architect should consult with all stakeholders to arrive at an ideal solution.
- When developing the facility layout, careful consideration should be given to the routes through the facility of staff, bodies and visitors. These routes should overlap as little as possible and there should never be a common entrance for bodies and staff or visitors.
- The room requirement sheets are presented in USER ROOM REQUIREMENTS of this document.
- Storage space for body lifts must be provided.
- Suitable sluicing facilities are required to be able to clean equipment and fabrics after completion of any work in the mortuary facility.
Mortuary Equipment Requirements
Equipment for storage and transportation of bodies should meet environmental hygiene standards.
For mortuary trolley design and supply, the SABS published standard CKS336:2013 Mortuary Trolleys is recommended. It should be noted that this is not a normative South African National Standard, and individual requirements may differ.
Body-cabinet selection and installation require the following considerations:
- Three-level body cabinets could be selected which have a single door to give access to all of the body trays, for instances where a separation between bodies is required. Alternatively, cabinets that provide a single door for access to all the body trays are acceptable.
- It is critical that bariatric (obese) bodies are catered for in each cabinet.The lowest-level tray should be designed for this purpose.
- Special consideration is to be given to the provision of capacity for storage of juvenile and infant decedents.The handling of these bodies is an especially sensitive and emotive issue, and separate storage in dedicated cabinets is recommended.
- Body lifts must be supplied to facilitate the loading of bodies into and removal of bodies from the cabinets. Body lifts help to preserve dignity when handling bodies, while at the same time making it easier and safer for mortuary personnel to handle bodies.
- A clear space must be provided in front of the body cabinets to allow for the placing of a corpse into the cabinets. It is recommended that there be at least a 3m clearance between the front of the cabinet and any fixed structure. This is to accommodate whatever means of conveyance is used to transport a corpse to the storage area and then load it into the cabinet.
- Due to the vast array of cabinets available on the market and the lack of an appropriate national standard, it is not yet possible to prescribe sizes for refrigerated cabinets in this guide.
- The required cabinet size is fundamental when designing a mortuary. Where space is not too limited and there are no indications that there may be cultural concerns relating to the storage of bodies together in a cold room, it is recommended that cold rooms be used.Cold rooms offer space savings when compared to cabinets.
- A temperature gauge must be installed close to the door of the facility to indicate the storage-space temperature. This gauge should have an alarm system connected to it to give a warning should there be an unacceptable rise in temperature in the storage space. Typically, if the temperature should rise more than 2?C above the set temperature,an alarm should be activated at a point that is manned at all times.
- Body cabinets and refrigerated rooms must be supplied with electrical power from the hospital’s essential services electrical supply.
- A slop hopper is to be provided to allow for the cleaning of the body preparation and autopsy areas, in particular after the completion of any work carried out in these areas.
- To allow for the rinsing of body parts and organs, during an autopsy procedure it is important that suitable basins be provided in close proximity to a downdraft autopsy table.
- Where there is a transition between “clean” and “dirty” areas, provision is to be made to allow for the cleaning of footwear in a “transitional” area. This helps prevent the transport of contaminants from dirty areas.
Movement Within a Mortuary
Movement of members of the public visiting the mortuary is to be restricted such that they do not have access to the body-preparation or autopsy areas.
- The facility must be available within the mortuary where body identification can be conducted in a private and dignified manner. This viewing area should consist of a body-display or layout room with an adjacent viewing room, where the body can be viewed through a curtained shatter-proof glass window.
- The requirement for a viewing and identification area also pertains to hospitals which outsource their mortuary services.
- The viewing room and visitors’ admin rooms should be designed such that counselling can be conducted in a pleasant environment for bereaved persons.
- The design of the viewing facility should allow adequate space for persons to view a body in a dignified manner.
- Direct access to the body-layout room from the viewing room is to be provided via a lockable door, to allow visitors access to the body.
- Ablution facilities are to be available to members of the public who are required to visit the mortuary complex
- Where a dedicated room, as described above, can not be allocated for placing a body for viewing purposes, the persons who are viewing a body should be given a private space for viewing the body through a curtained shatter-proof glass window, as a minimum.
- Adequate facilities to accommodate at least 7 visitors are to be provided.
- Staff access to the mortuary facility is to be separate from the general public.
- Mortuary staff change rooms should be provided with secure lockers for storage of street garments, lab coats, personal protective equipment and valuables.
- Mortuary staff may have completely separate ablution facilities from those used by the general public requiring access to the mortuary facility.
- In a free-standing mortuary building, the delivery to and removal of bodies from the facility may be via the same access point to the building.
- A mortuary that forms an integral part of a hospital will require separate routes for receiving bodies and the subsequent removal thereof.
- In the unusual event that a body arrives from outside the hospital, the normal route of removal should be used for receipt of the body.
- A clear distinction is to be made between “clean”,” “dirty” / “wet” and “transitional” areas. This is best achieved by creating a physical “RED LINE” on the floor indicating the separation of these areas, with “yellow lines” used to demarcate “transitional” areas. Receptacles for the collections of dirty clothing, etc, must be made available at the transition area from dirty to clean areas and in change rooms.
- A well-drained facility for washing vehicles which have been contaminated with decomposed bodies or body fluids should be provided in an enclosed area, near to the mortuary.
- Mortuary staff change rooms should be provided with secure lockers for storage of street garments, lab coats, personal protective equipment and valuables.
Services Required
- Hygienic floor drains that are resistant to corrosion from blood and chlorine should be provided in all “wet areas” of the mortuary and should be directly connected to the sewer system. These areas include body preparation, autopsy space, etc. These areas require thorough cleaning after every procedure, using large quantities of water and decontaminating and disinfecting chemicals and soaps.
- Sluicing facilities are to be provided in both the body-preparation and autopsy areas if they are not a common area.
- Open floor channels should be avoided. Where this is not possible, these should be covered by durable, flush-fitted stainless steel grids.
- No sewer connections external to the mortuary services should be made to the line between the wet area drains and the main sewer system in order to prevent backflow to other areas.
- The provision of hot and cold water in the facility is imperative, with all basins, sinks, ablution areas and autopsy tables being provided with both.
- Anti-backflow devices should be fitted to the water-supply lines serving mortuary table faucets to prevent backflow should supply water pressure fail.
- Electricity supply to the mortuary – particularly for refrigeration purposes – is to be provided from the essential supply system for the hospital. Alternatively, a back-up generator is to be supplied to allow for the maintenance of required temperatures in the cooling/freezing facilities in the mortuary.
Biological Safety
- A Level 3 containment area (BSL3 designation - R178-2012) is required for any post-mortem area for decomposing bodies.
- Level 3 containment areas shall have restricted access and shall be separated from regular traffic flow routes.
- All doors opening into the Level 3 containment areas shall be appropriately labelled with biological safety hazard signage.
- Access to the Level 3 containment areas shall be through dedicated ventilated airlocks. A pressure differential of minimum +15Pa shall be maintained for the airlock relative to the BSL3 area. This pressure differential is relevant for when the doors are closed only. Room pressure differential gauges are to be fitted at the entrance to the Level 3 containment area.
- Airlock doors shall be interlocked such that only one door can be opened at a time, thereby preventing direct passage between the corridor and the Level 3 containment area.
- It is recommended that a transfer hatch be created for the transfer of goods between areas with differing biosafety-level classifications. This device shall be designed to preserve the integrity of the containment system and the mechanical ventilation design.
- Air exhausted from Level 3 containment areas should be safely discharged to the outside with no chance for re-entrainment or contamination of other indoor spaces.
- Exhausts from Level 3 containment areas should be vented beyond the building recirculation zone or at more than 3m above the roof level at 15m/s.
- Where such measures are not possible, exhaust air shall be EN1822 H13 HEPA filtered.
- Exhausts from Level 3 containment areas should include anti-backflow devices.
- Exhaust from any post-mortem area for decomposing bodies should include odour control measures.
Finishes to Floors and Walls
- Walls and floor coverings within a mortuary should be easily cleanable and impervious to liquids and staining.
- Floors are to be of such a nature that they are not easily damaged by wheeled items that are moved over them.
- Vinyl floor coverings are not considered to be resilient enough for this purpose.
- Epoxy floor coverings are preferable, as these are easily maintained and do not have joints in them where liquids can accumulate to become a health risk.
- Corners between walls and floors shall be coved to facilitate the cleaning of these areas. These coving details should be solid and continuous without hidden formwork and cavities.
- Walls are to be coated with hard-wearing and washable materials/paint with provision made for trolley bump-rails along walls exposed to high traffic. Wall coatings shall be impervious to damage from trolleys and mobile equipment.
- Materials such as vinyl sheeting should not be used to cover walls in wet areas. The risk of growth between the sheeting and the wall presents a health hazard to personnel working in the mortuary wet areas.
- Due to the potential presence of water on the flooring, it is essential that flooring be non-slip.
- Refer to the room requirement sheets herein and the IUSS:GNS Materials and finishes guidance documents for further information.
- Surface-mounted services should be avoided to ensure smooth and washable surfaces. Where surface mounting of piping is unavoidable, this piping should be mounted on batons, such that the space behind the piping is readily accessible for cleaning.
Autopsy Equipment/Fixtures
- Equipment for the storage and transportation of bodies should meet occupational and environmental hygiene standards.
- In the majority of instances, a downdraft autopsy table is required within a hospital mortuary facility. This table should be one that is designed in such a way that there is a hot and cold water supply that is integral to table installation, as well as a drainage system that can automatically drain water/waste from the table to the sewer system of the facility.
- The autopsy table should have an integrated ventilation extraction or “downdraft” system in order to entrain noxious odours and infectious material that may emanate from a body. This can function to minimise the spread of any airborne pathogens from the body.
- Adequate stainless steel washing basins (at least one per autopsy table) must be provided in close proximity to the autopsy table for the use of personnel working in the facility.
- Electrical power must be provided from a 5 amp IPX5 waterproof single-socket outlet near the autopsy table to allow for the safe use of any electrical equipment that may be required during an autopsy.
- Lighting quality over the autopsy table must be exceptionally good. Refer to the lighting requirements specified in the room-requirement sheets herein and the IUSS:GNS Building engineering services guidance document for specifications.
- Adequately sized worktops must be provided along the walls of the autopsy area for equipment and specimens prior to storage.
- It is recommended that working surfaces of at least 500x2500mm be provided per autopsy table.
- A balance table for a bench-top scale is required. The scale can be either permanently mounted on the work surface or stored in the autopsy equipment store.
- A platform scale for measuring the weight of an entire body prior to any possible dissection/autopsy work being conducted is to be accommodated.
- Lockable cabinets are required for the storage of autopsy equipment, as well as for any personal protective equipment morticians or medical examiners may require.
- Trolleys for the conveyance of bodies must be provided in the mortuary and adequate provision for the cleaning and storage of these units must be available.
- The use of wood, such as for wooden doorframes, is not recommended and is not permitted in wet areas
- Stainless steel bump-rails or plates should be fitted in areas prone to damage from trolleys. These devices shall be fitted such that they do not affect the integrity and cleanability of the walls and floors. These devices shall not create crevices or gaps which could harbour pathogens or create a hygiene problem. Welded stainless steel sections shall be stainless steel Grade 316L
Ventilation
- Mortuary areas require good ventilation. The exhaust air is to be discharged to the atmosphere such that it cannot be drawn back into the mortuary, any other ventilation inlet, or any indoor portion of the hospital.
- All external ventilation openings should be fly- and vermin-proof.
- Exhausted air must not pose a hazard to any person who is outside the mortuary. (See room-requirement sheets) Air exhausted from clinical areas should be safely discharged to outside with no chance for re-entrainment or contamination of other indoor spaces. Where these precautions are by no means possible, exhaust air shall be EN1822 H13 HEPA filtered.
- Sufficient ventilation is required for controlling noxious odours present in mortuaries and should also provide a means of protection to personnel working in the facility from possible airborne infections originating from corpses.
- Tuberculosis, Hepatitis and HIV are among the most regularly encountered diseases in mortuaries in South Africa and, as such, the spread of these pathogens beyond the mortuary, via a ventilation system, must be avoided. Airborne-infection control is of particular concern and must be integrated into the design of the ventilation system. Airborne-contamination control principles must be applied to the design of the ventilation of high-risk. Refer to the IUSS:GNS Building engineering services guidance document for further guidance on airborne-contamination control principles.
- The ventilation system must be designed such that airborne pathogens that may be present in the body-holding area and autopsy room do not contaminate the remainder of the mortuary facility.
- No recirculation of air extracted from the clinical areas is permitted.
- Air from public areas, with the exception of viewing rooms, may be recirculated where this is in accordance with the National Building Regulations.
- Exhaust ventilation is to be designed in such a manner that this extracts more from the areas with the highest risk of infection, while more “clean” air is to be supplied into the lower-risk areas. This is to create a pressure cascade with cleaner areas being at a relatively higher air pressure than dirty areas.
- Supply air registers should be at a high level and the extraction registers should be at a low level. The bottom of low-level extraction grilles shall not be between 300mm and 500mm above the finished floor level of the room from which the extraction is taken. Low-level air-register positions shall consider locations of water points and potential splashing during washing.
- Low-level extraction grilles shall have removable faceplates to enable easy duct cleaning.
Air Conditioning
- The mortuary and autopsy area must have a temperature maintained between 20˚C and 21˚C.
- Public areas must be kept at a constant temperature between 23˚C and 25˚C.
- Air extracted from the mortuary and autopsy area may not be used for energy recovery or recirculation.
Refrigeration Equipment Design and Installation
- All heat-rejection equipment associated with refrigeration in the body-storage facilities must be located on the outside of the mortuary, in a well-ventilated space at the rear of the fridge(s). Compressors installed on top of body cabinets on the inside of the mortuary are not acceptable. Heat build-up within the mortuary, as a result of this type of arrangement, potentially leads to equipment failure.
- Refrigeration equipment components that require regular maintenance interventions should not be situated within the confines of the mortuary. Refrigeration technicians should not be required to climb onto or over any equipment to carry out any maintenance work. It is preferable to have refrigeration equipment situated in a separate and ventilated area to the rear of the body cabinets. The designer is to refer to the selected heat-rejection equipment’s installation manual to determine free space and ventilation openings required around this equipment since these details can vary between system types.
- Gauges indicating the temperature within the body cabinet must be clearly visible above the door of the unit in order that this can be readily monitored.
- The acceptable average temperature within a normal body cabinet or refrigerated room is between 2.0˚C and 6˚C. In instances where a body has to be kept for an extended period of time a cabinet temperature of at least -20˚C is required.
- In facilities where large quantities of bodies are kept, cold rooms for the storage of multiple bodies on trays are recommended.
- The materials used for the construction of the units are to be of stainless steel to facilitate cleaning and long-term maintenance of the equipment. Grade 316 stainless steel (18/10) is preferable over Grade 304 (18/8), as it offers better corrosion resistance.
- For welded stainless steel construction, Grade 316L or similar is required.
- If a facility is required to collect and retain forensic evidence (e.g. clothing of decedents), refrigeration equipment should be provided for the preservation of these samples. Preferably this equipment should be placed in an area where it can readily be secured from unauthorised access and tampering.
Security Arrangements
- Due to the medical and legal nature of the contents of a mortuary, it is essential that a mortuary has good access control and security systems.
- Theft from mortuaries should be forestalled by, inter alia, constantly monitoring all entrances and preventing free access to mortuary areas. This is especially important for body-storage areas. Access card or tag systems are open to misuse and are not an appropriate access-control measure. Combinations of tag and biometric access control systems are recommended.
- Door closers with a “hold-open” mechanism should be installed on the mortuary room doors. This enables doors to close automatically with normal traffic, but can also be held open when moving equipment or trolleys through. “Crash”-type doors should be avoided as these are not easily cleanable and are subject to damage and abuse.
- It is recommended that a timed alarm be fitted to doors to ensure that they are closed shortly after any entrance or exit. This is to militate against keeping doors open with some form of door stopper.
- Body cabinets are to be fitted with locks to prevent the unauthorised opening of these units to forestall the theft of any personal items of the deceased.
- In instances where historical problems relating to unauthorized entry into mortuaries is evident, it is recommended that closed-circuit TV systems be installed to help in monitoring and securing the facility.
OPERATION
Objectives
The project planning, design, construction and commissioning should aim to provide:
- safe, secure and functional environment for visitors and staff;
- low capital and ongoing operating costs (service, staffing and maintenance);
- an environmentally appropriate design solution; and
- a fully accessible, inclusive environment.
Health and Safety
In light of the above, it is essential that every effort is made to ensure that personnel working in the mortuary are provided with all required personal protective equipment (PPE), as this is essentially an area where pathogens could be present and present a health risk to staff. The following items should be available to staff as a minimum:
- Rubber aprons (or similar impervious material)
- Latex gloves (or similar impervious material)
- Mesh gloves in facilities where post mortems are performed
- Disposable gowns
- Safety glasses or full-face visors.
- Waterproof footwear
- Face masks
- Respirators with the appropriate filters must be available for use in high-risk situations.
- Storage space for PPE
No one should be permitted to enter the body storage and preparation areas without donning appropriate gowns and footwear.
Maintenance
When designing the facility, every effort must be made to limit the amount of maintenance that would be necessary to keep it in good condition. Seamless surfaces for walls and floors are critical, as this will reduce ongoing maintenance costs. The following minimum requirements should be complied with:
- Seamless floor coverings required
- Continuous coving with radius >50mm required between floors and walls.
- No sharp corners on any work surfaces that could injure people working in the area.
- Ceilings to be readily cleanable.
- Work surfaces are to be impervious to liquids and resistant to staining and corrosion.
- Refer to the room-requirement sheets herein and the IUSS:GNS Materials and finishes guidance documents for further information on the general requirements for materials and finishes.
- All equipment requiring calibration, such as fridges and scales, are to be attended to on an annual basis or when it is suspected that they are defective in respect of their expected/intended performance
ROOM USER REQUIREMENTS
| Accomodation Shedule | |||||
| Room Name | Service Description | Area
(m²) |
Min. Ceiling Height
(m) |
Occupancy
(Persons) |
Nominal Utilisation per day
(hours) |
| Ablution areas | Ablution areas- male and female
One WHB per WC or urinal |
3 (per cubicle) | 2.8 | 1 | 4 |
| Shower facilities | Shower facilities- male and female | 3 (per cubicle) | 2.8 | 1 | 2 |
| Changing room | Staff changing room - lockers to be provided | 8 | 2.8 | 2 | 2 |
| Storage space | Equipment and PPE storage space | 8 | 2.8 | 1 | 1 |
| Offices | Office space- interview, body receiving, pathologist | 9 | 2.8 | 2 | 8 |
| Body/bier room | Area where a body can be laid out for viewing and identification | 9 | 2.8 | 1 | 8 |
| Viewing room | Viewing room- external to body-layout area | 9 | 2.8 | 4 | 1 |
| Autopsy room | Autopsy facility- Autopsy table with water supply and discharge and extraction ventilation. WHBs and stainless steel working surfaces | 27 | 2.8 | 3 | 3 |
| Room Service Sheet | ||||||||||
| Room Name | Temp
(°C) |
Ventilation
(AC/h) |
Ventilation
Type |
Pressure Relative to
Ambient |
Wet Services | SSO
400V |
SSO
230V |
Task Illuminance
(lux) |
Data Points | Colour Rendering
(Ra) |
| Reception area | 22-25°C | 2 | Forced supply | = | 0 | 0 | 100 at floor level | 0 | 80 | |
| Visitors ablution areas | 22-25°C | 15 | Forced extraction | - | WC, WHB | 0 | 0 | 150 at floor level | 0 | 80 |
| Public waiting area | 22-25°C | 2 | Forced supply | + | 0 | 0 | 100 at floor level | 0 | 80 | |
| Offices | 22-25°C | 2 | Forced supply/ recirc. | = | 0 | 2 | 300 at desk level | 1 | 80 | |
| Circulation Spaces | 22-25°C | 10 | Forced supply/ recirc. | = | 0 | 0 | 200 at floor level | 0 | 80 | |
| Viewing room | 22-25°C | 2 | Forced supply | + | 0 | 0 | 100 at floor level | 0 | 80 | |
| Layout room | 20-21°C | 2 | Forced extraction | - | WHB | 0 | 0 | 300 at table level | 1 | 80 |
| Storage space | 22-25°C | 4 | Forced supply | = | 0 | 1 | 200 at floor level | 0 | 80 | |
| Mortuary | 20-21°C | 12 | Forced extraction | - | WHB, FD | 0 | 1 | 200 at floor level | 0 | 80 |
| Mortuary plant area | n/a | n/a | Natural ventilation | = | 1 | 1 | 150 at floor level | 0 | 80 | |
| Autopsy table | 20-21°C | 20 | Forced extraction | - | CW Faucet | 0 | 1 | 5200 at table level | 0 | 90 |
| Autopsy room | 20-21°C | 20 | Forced extraction | - | WHBs, FD | 0 | 2 | 500 at floor level | 1 | 90 |
| Changing room | 22-25°C | 15 | Forced extraction | - | WHB | 0 | 1 | 150 at floor level | 0 | 80 |
| Staff ablution areas | 22-25°C | 15 | Forced extraction | - | WHB, WC | 0 | 0 | 150 at floor level | 0 | 80 |
| Shower facilities | 22-25°C | 15 | Forced extraction | - | CW + HWFaucet | 0 | 0 | 150 at floor level | 0 | 80 |
| Room Finishes | |||||||
| Room Name | Floor
Material |
Wall / Floor Interface | Walls
Finish |
Ceiling
Finish |
Glazing
Type |
WHB | Doors
Type |
| Ablution areas (all) | Jointless vinyl sheet | Skirting coved and finished as per floor | Ceramic wall tiles with epoxy grout | Acoustic Ceiling tiles | Obscure laminate safety glass | 1 per WC or urinal | Solid wood with galvanised steel or stainless steel sheet trolley plates |
| Public waiting area | Jointless vinyl sheet | Coved vinyl skirting | Washable acrylic paint | Acoustic Ceiling tiles | Clear laminate safety glass | 0 | Lockable glazed entrance door |
| Changing room | Jointless vinyl sheet | Skirting coved and finished as per floor | Washable acrylic paint | Washable acrylic paint | Obscure laminate safety glass | 0 | Solid wood with galvanised steel or stainless steel sheet trolley plates |
| Storage space | Jointless vinyl sheet | Skirting coved and finished as per floor | Washable acrylic paint | Washable acrylic paint | Clear laminate safety glass | 0 | Solid wood with galvanised steel or stainless steel sheet cladding |
| Offices | Jointless vinyl sheet | Coved vinyl skirting | Washable acrylic paint | Washable acrylic paint | Clear laminate safety glass | 0 | Solid wood |
| Body Room | Self- levelling epoxy | Skirting coved and finished as per floor | Washable acrylic paint | Washable acrylic paint | Clear laminate safety glass | 0 | Solid wood |
| Viewing Room | Self- levelling epoxy | Skirting coved and finished as per floor | Washable acrylic paint | Washable acrylic paint | Clear laminate safety glass | 0 | Solid wood |
| Autopsy Room | Self- levelling epoxy | Skirting coved and finished as per floor | Washable acrylic paint | Washable acrylic paint | Obscure laminate safety glass | Min 1 per autopsy table | Solid wood with galvanised steel or stainless steel sheet cladding |
| Circulation Spaces | Jointless vinyl sheet | Coved vinyl skirting | Washable acrylic paint | Washable acrylic paint | Clear laminate safety glass | 0 | |
EXAMPLES AND CASE STUDIES
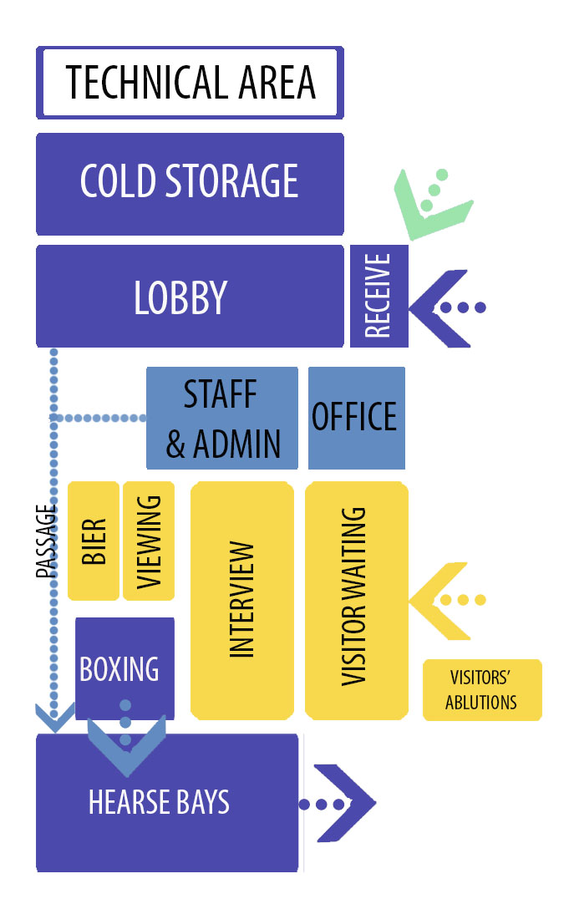
A Small Mortuary Attached to a Hospital
The figure below demonstrates the relationships between the zones within the mortuary. In this example, it is evident how visitors are managed and kept out of the working portions of the mortuary through segregation in the internal layout. The process flow of the bodies into, through and out of the mortuary has been well considered in that the flow is linear with bodies entering the mortuary at one end of the facility and exiting at the other.
Unfortunately, the restrictions presented by the location of the mortuary, as can be studied in the figure above, has forced the design into a number of compromises relating to the external flow and access to the mortuary. Staff access is quite severely compromised in being through the mortuary lobby. This mortuary lobby, in the absence of a dedicated preparation room, has the potential of being used as one. This arrangement may impact negatively on the dignity of some staff, the dignity of the deceased, and mortuary security.
Visitors’ access to the mortuary and their adjacent toilets is near the hearse bay and turning areas. There is no natural screening of this entrance from the activities in the hearse bay and it is not inconceivable that visitors may inadvertently wander into the wrong area and be exposed to operational activities not appropriate for the bereaved.
The door sizes of the body storage rooms seem too small for the easy passage of a body trolley when compared to the double doors made available for the passage of the body from there through the remainder of the facility. Door size selection should not be limited by the fact that these are cold room doors. Where doors are too small for free passage of trolleys and porters, the doors’ service life would be severely shortened and any savings made on the door selection would be lost to maintenance or retrofitting an improved solution. The access to the technical area for maintenance of the refrigeration equipment in this example meets the recommendations. Here technicians do not need to enter the mortuary to perform the majority of their work and these areas are quite well separated from the admin and visitors’ areas.
A Large Mortuary with Autopsy Facilities
The layout below shows a standardised mortuary design. This is a large facility with autopsy capacity. The zoning diagram below has been presented in order to promote an understanding of the interrelationship between the various functional parts of the mortuary. Considering the entrances shown, it is clear that the designer has made an effort to screen the visitors’ entrance from the hearses’ entrance. The staff entrance is also well positioned. The staff ablution facilities and showers are located between the clinical areas and the admin areas. This arrangement encourages good segregation and gowning practice when moving between the mortuary activities and external movement. The staff and visitors’ access positions are located well away from the working clinical areas of the mortuary and are also relatively remote from each other. This aids in improving security as it discourages the staff and visitors from using the wrong entrances and thereby assists in identifying persons who are present in areas where they do not belong. This design doesn’t have a dedicated body prep area and it is assumed that the weighing and measuring area is therefore used for this purpose. The large sliding doors of the cold room in this example can be compared to the cold-room doors in the small mortuary layout above as an indication of what the door size should be like to enable easy passage. The layout in this example does not provide for a dedicated exit yard and bodies and hearses entering and leaving the facility do so through the same entrance. This arrangement increases the potential for mistakes in body handling. The common use of the bier room as access to the ID room seems to be a compromise resulting from the limited space provided for these rooms.
Another Large Mortuary with Autopsy Facilities
The example in the figure below resolves many of the compromises in the arrangement of the bier rooms and ID/viewing rooms’ available space, discussed in the previous example.